A 75-Word Limit Shouldn't Take Five Tries
We asked a language model to answer patient questions under simple constraints. It matched the word count. It didn't match the writing.
Ask a language model to answer a patient’s question from their medical record. Simple enough. Now add constraints: ground every claim in a specific sentence from the clinical note. Keep it under 75 words. Use past tense for events during hospitalization, present tense for prognosis. Match the style of a clinician writing for a lay reader.
Each of these instructions is straightforward on its own. Stack them together and the model starts failing in ways that standard evaluation metrics don’t capture.
The 75-word problem
We built a system for the ArchEHR-QA 2026 shared task, which evaluates grounded question answering from electronic health records. The task requires a model to identify which sentences in a clinical note support the answer, generate a natural-language response under 75 words, and align each answer sentence to its evidence.
The simplest constraint was the hardest to enforce. On the development set, 85.9% of outputs met all format and length requirements on the first attempt. On the test set, that dropped to 64.3%. Word count violations accounted for 95% of all test errors. Not citation errors. Not format errors. The model couldn’t count to 75.
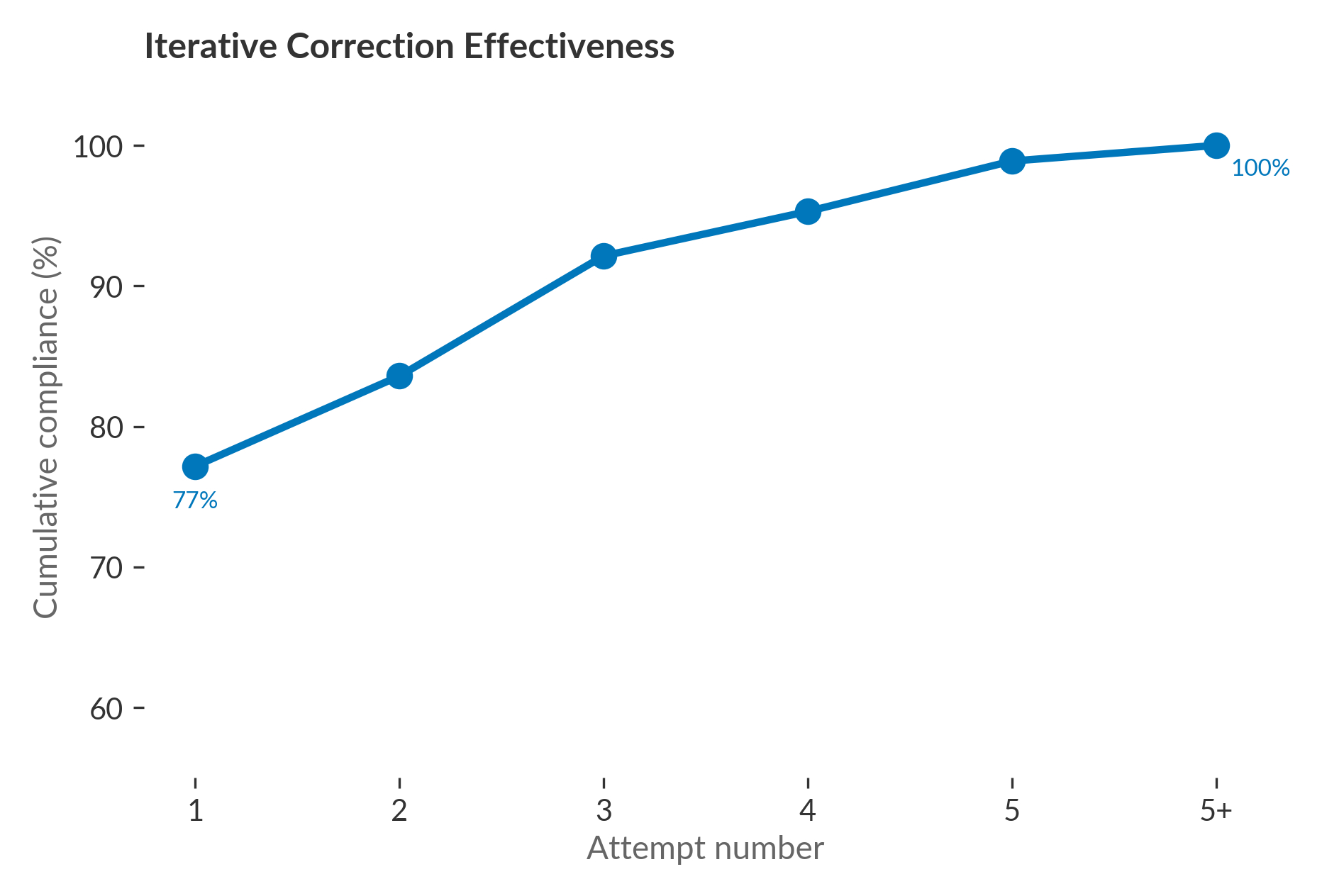
We fixed this with an iterative correction loop: when an output violated a constraint, we told the model exactly what was wrong and let it retry, up to five times. The loop achieved 100% compliance on both sets. But the fact that it was necessary at all is the point. A model that needs five attempts to meet a word limit it was given in the original prompt is not following instructions. It’s being corrected into compliance.

What the metrics missed
The compliance loop solved the format problem. It did not solve the style problem.
Our system matched clinician-authored answers on word count (72.7 vs. 73.5) and sentence count (4.45 vs. 4.75). Neither difference was statistically significant. By the most obvious measures, the outputs looked like clinician writing.
They weren’t. We computed 45 linguistic features across six categories and compared model outputs to clinician references
These answers are intended for patients. A response that is factually correct, properly grounded, and within the word limit can still fail its purpose if the patient can’t understand it. The standard evaluation metrics (BLEU, ROUGE, BERTScore, MEDCON) did not flag this gap. Length matched. Style didn’t.
The retry loop repaired what the benchmark could see. It did not repair what the communication task actually required.
More instructions, worse results
The natural question is why. The model was explicitly instructed to write in plain language. It was given style guidance, tense rules, and a word limit. Why did it follow the word limit (eventually) but not the register?
Some researchers call the failure mode “cognitive overload.” LLMs do not have cognition. What happens is better described as constraint interference: the model satisfies whichever instruction is most explicitly reinforced and underperforms on the rest. Word count is easy to verify and correct. Register is not. In our results, that asymmetry is exact: every word-count failure triggered a correction attempt; no equivalent mechanism existed to detect or retry a register failure.
You can split the task. That doesn’t solve the problem.
We tested whether separating the competing objectives would help. After the submission deadline, we built a three-step rewrite variant: (1) generate an unconstrained answer grounded in the evidence, (2) rewrite it for clinical register, (3) enforce the word limit as a separate call.
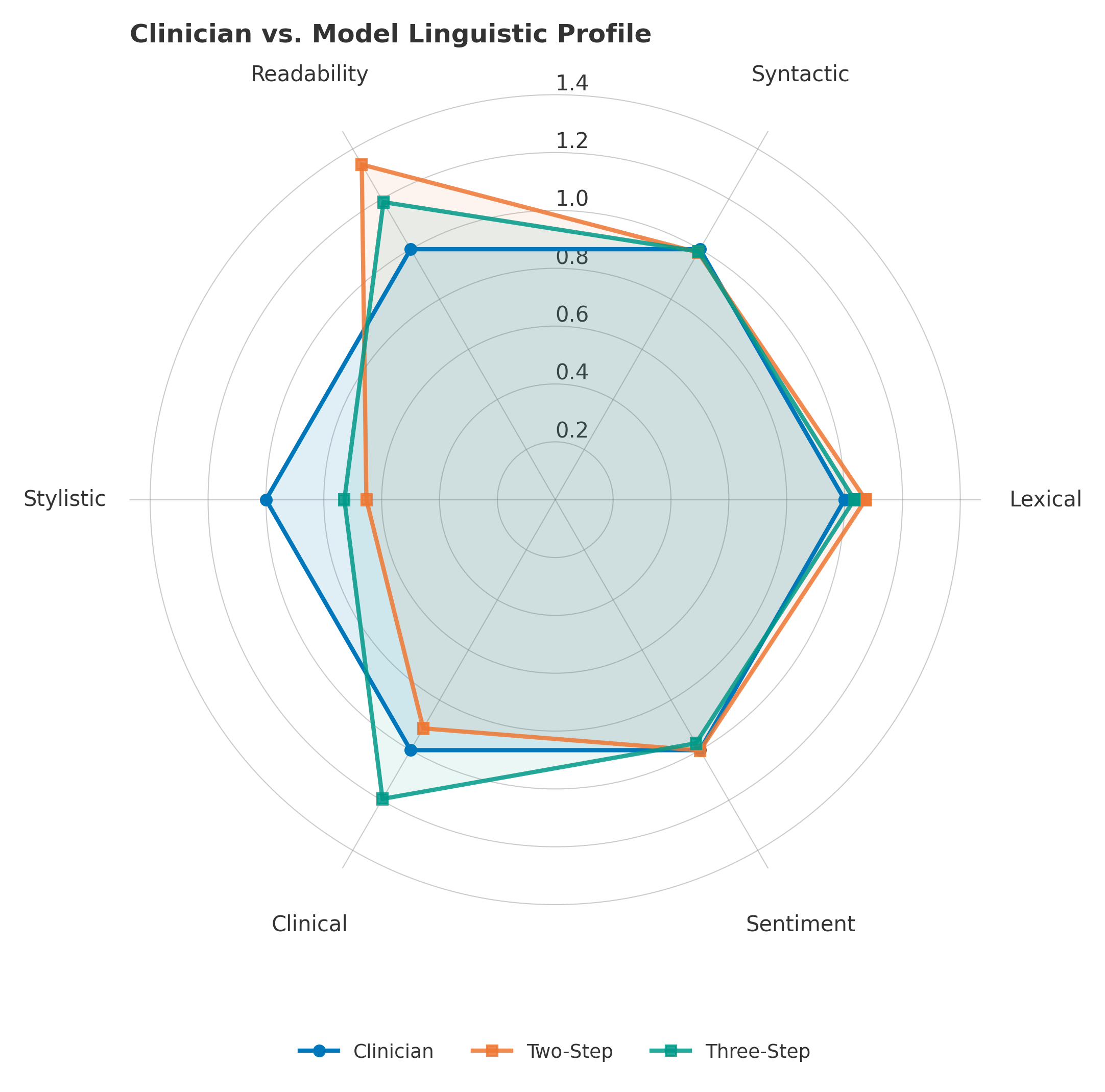
The decomposed pipeline reduced the linguistic distance to the clinician reference from 0.519 to 0.381 and improved the answer generation score (Subtask 3 Overall) by approximately two points on the development set. Readability moved closer to clinician levels. The cost: 9.5x latency and a three-stage orchestrated pipeline in place of a single model call.
That cost is the point. The improvement didn’t come from a better model or a smarter prompt. It came from decomposing the problem, routing each subproblem to a separate call, and engineering the handoffs. At some point you’re not using a language model to generate answers. You’re building a scaffold around one to compensate for what it can’t do reliably. The benchmark credit belongs to the pipeline, not the model.
64.3% is the real number
Our system achieved 100% compliance after correction. That sounds like success. But 100% compliance after five attempts is not the same as 100% compliance on the first attempt. The first number means the scaffold works. The second number means the model works. On the test set, the model’s first-pass compliance was 64.3%. That is the real number.
In clinical settings, the tolerance for errors approaches zero. If a system cannot demonstrate near-zero error rates on simple, verifiable constraints like word count, it cannot be trusted with harder, less verifiable ones like reading level, tone, and clinical accuracy. The easy constraints are the lower bound. If the model fails there, everything above it is suspect.
The workarounds exist. Decompose, correct, verify, repeat. Each layer of scaffolding is an admission that the model alone is not reliable enough. When the benchmark reports performance on a system like this, the credit belongs to the scaffold, not to the model. In clinical applications, the difference between a reliable model and a reliable scaffold is the difference that matters.
Enjoy Reading This Article?
Here are some more articles you might like to read next:
Subscribe to be notified of future articles: